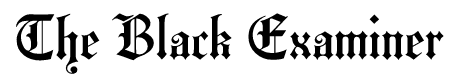A recent study in Uganda shows that well-constructed housing reduces malaria transmission. The research, conducted between November 2021 and March 2022, involved data from over 4,800 children aged 2 to 10 years across 3,518 households near 64 health facilities in 32 districts.
Houses in the study were categorized as ‘improved’ if they featured synthetic walls and roofs with closed or absent eaves, and ‘less-improved’ if they had other construction types. The study found that children living in improved houses had a 58% lower chance of having malaria parasites (adjusted odds ratio = 0.42, 95% CI 0.33–0.53, p < 0.0001) compared to those in less-improved houses.
At the community level, areas with over 67% of improved houses exhibited a 63% lower parasite prevalence (adjusted prevalence ratio 0.37, 95% CI 0.19–0.70, p < 0.0021) and a 60% lower malaria incidence (adjusted incidence rate ratio 0.40, 95% CI 0.36–0.44, p < 0.0001) compared to communities where less than 39% of houses were improved. This association was assessed using multivariable fractional response logistic regression and multivariable Poisson regression, controlling for various community-level factors such as wealth index, precipitation, and vegetation.
The study, embedded within a larger trial (LLINEUP2), also highlighted the broader context of malaria control in Africa, where traditional vector control methods like long-lasting insecticidal nets (LLINs) and indoor residual spraying (IRS) have shown limitations due to insecticide resistance and gaps in coverage. The efficacy of improved housing in reducing malaria burden complements these methods, offering a sustainable, non-insecticidal intervention.
Methodologically, the research utilized enhanced surveillance at Malaria Reference Centers (MRCs) across Uganda, employing cross-sectional surveys to enumerate households and collect detailed data on housing types, socio-demographic factors, and malaria outcomes. Data analysis involved sophisticated statistical models to account for individual and community-level variables, demonstrating robust associations between housing quality and malaria indicators.
Researchers underscored the potential of improved housing as a non-insecticidal approach to complement existing vector control strategies like LLINs and IRS. They noted that well-built houses serve as a physical barrier against malaria vectors, limiting their entry and reducing exposure to infectious mosquito bites. Investing in housing improvements could offer substantial benefits in malaria control efforts, particularly in regions where traditional housing with mud walls and thatched roofs predominates.

Despite progress in malaria control over the past two decades, recent years have seen a stall in these gains, driven by factors such as inadequate coverage of control tools, disruptions from COVID-19, and emerging resistance to drugs and insecticides. The study suggests that investing in improved housing could be a vital strategy in revitalizing efforts against malaria in Africa. Given the increasing population and rapid urbanization in Africa, the findings advocate for integrating better housing construction into public health strategies. Improved housing not only reduces malaria but also contributes to overall health and well-being.